La mejor atención. Sin límites.
En Philips tenemos el compromiso de ofrecerle las soluciones a todas las respuestas que necesita en el momento adecuado. Redefiniendo la experiencia de la medicina de la mano de la atención al paciente con el firme compromiso de liderar el futuro de la atención médica con una amplia cartera de soluciones.
Si hoy en día la salud no tiene límites, la sanidad tampoco debería.
La mejor atención. Sin límites.
En Philips tenemos el compromiso de ofrecerle las soluciones a todas las respuestas que necesita en el momento adecuado. Redefiniendo la experiencia de la medicina de la mano de la atención al paciente con el firme compromiso de liderar el futuro de la atención médica con una amplia cartera de soluciones.
Si hoy en día la salud no tiene límites, la sanidad tampoco debería.
¿No quiere perderse nuestras últimas novedades?
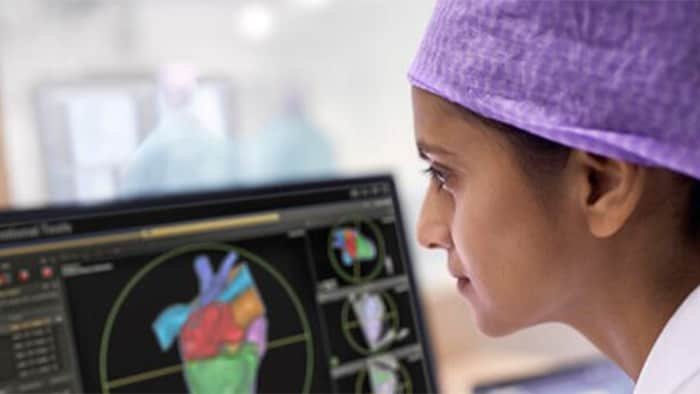
Cardiología
Los cuidados cardiacos mejorados comienzan con diagnósticos definitivos, procedimientos innovadores y gestión de pacientes personalizada
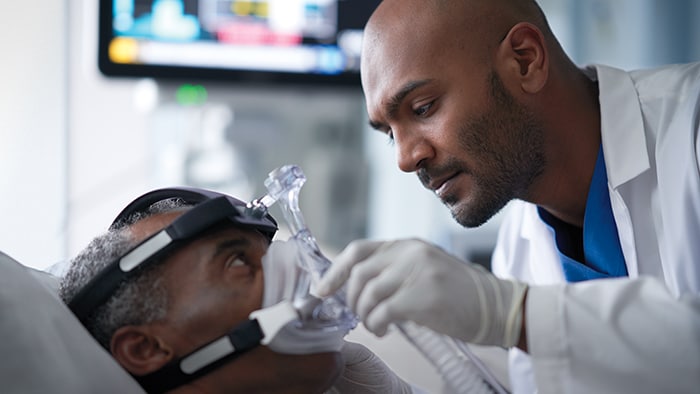
Cuidados Respiratorios
Conectamos el hospital y el hogar, y facilitamos el intercambio de datos entre médicos y pacientes para proporcionar un tratamiento personalizado.

Consultoría
Afrontamos el reto de proporcionar una atención de calidad a un coste menor, al tiempo que aumentamos la satisfacción del paciente y del personal.
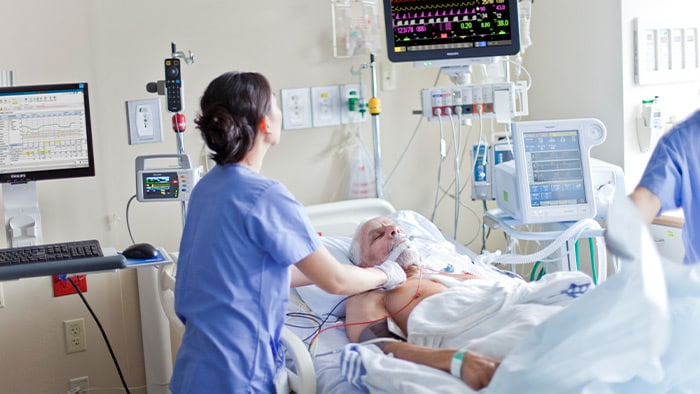
Cuidados Críticos
La atención al paciente no se detiene. Desde el ingreso hasta el alta, los latidos, la respiración, la atención del paciente y el entorno cambian, mientras que los conocimientos vitales evolucionan..

Informática Clínica
Ayudamos a nuestros clientes a adaptarse al mundo en evolución de la atención sanitaria y a avanzar en la transformación digital de la salud.
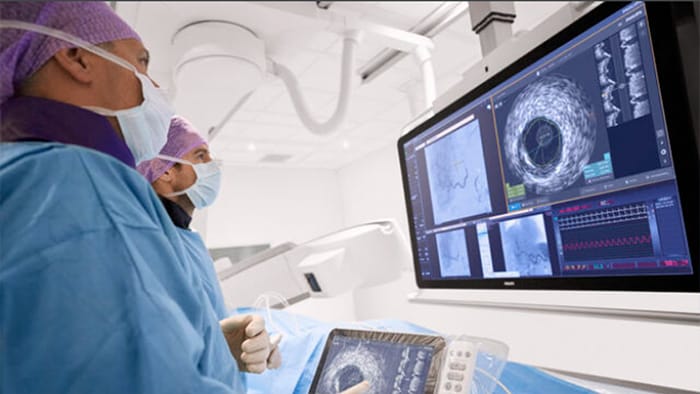
Terapia Guiada por Imagen
Sistemas de adquisición de imágenes intervencionistas, dispositivos inteligentes, software y servicios
Radiología
Soluciones integrales que proporcionan servicios de adquisición de imágenes de alta calidad a los profesionales sanitarios

Operaciones Hospitalarias
Servicios diseñados para proporcionar el nivel de apoyo adecuado a los clientes para satisfacer sus necesidades operativas hospitalarias.
Cuidado cardiovascular
Nuestras soluciones de atención cardiovascular ayudan a los profesionales de salud a satisfacer las demandas de una creciente población con enfermedades cardiovasculares, dentro y fuera del hospital.
Monitorización
Diseñados para permitir la visibilidad del estado de un paciente prácticamente en cualquier momento y lugar, nuestros productos de monitorización de pacientes y herramientas de apoyo a la toma de decisiones clínicas ofrecen una experiencia de usuario más conectada a la vez que agilizan el flujo de trabajo.
Obtención de imágenes
Desde la Tomografía Computarizada y la Resonancia Magnética hasta los rayos X y los ultrasonidos, toda nuestra cartera de productos de diagnóstico por imagen tiene como objetivo ofrecer a los profesionales sanitarios la imagen adecuada en el momento oportuno, para facilitar un diagnóstico más rápido y seguro.
Informática clínica
Nuestras soluciones de informática clínica tienen como objetivo transformar grandes cantidades de datos clínicos en información integrada que guíe la atención del paciente en toda su empresa.
Aplicaciones clínicas
Para resolver algunos de los retos clínicos más importantes en la atención al paciente, ofrecemos una gama de aplicaciones clínicas que reúnen hardware, software, tecnologías y servicios que pueden adaptarse a las necesidades de su organización.
Consultoría & Servicios
Nuestros equipos aportan una gran experiencia en muchos aspectos de la atención médica, desde la excelencia clínica, la optimización del flujo de trabajo y la experiencia del paciente, hasta el mantenimiento de equipos y la capacitación y educación del personal.
Salud de la población
Nuestros programas de gestión de la salud de la población ayudan a impulsar la mejora de la calidad, el aumento de los ingresos y la transformación del negocio para los proveedores, los sistemas de salud, los empleadores y los pagadores en una plataforma única y completa
Tecnologías de diagnóstico
Los avances digitales en la atención sanitaria son muy prometedores para mejorar la velocidad y la fiabilidad del diagnóstico, así como la vía más adecuada para el tratamiento.


